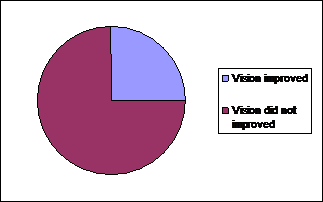
Fig. 1: Three months patching
result.
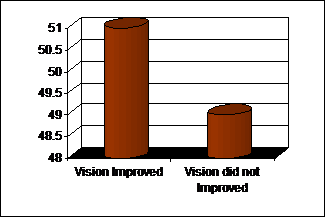
Fig. 2: Six months patching
result.
vision improved in 51% and did not improve in 49% (Figure 2).
Graphical representation
showed that the results of vision improvement were comparatively less in
strabismic and anisometropic amblyopia with six months patching treatment as
shown in figure 3.
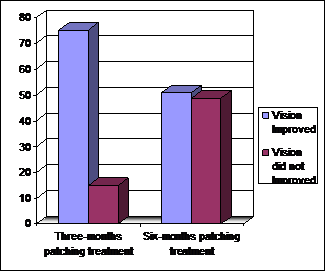
Fig. 3: Three
and six months patching result.
DISCUSSION
This
comparative study assessed the strabismic and anisometropic amblyopic patching
therapy among the age group 4-10 years. Correction of refractive error with
spectacles along with the patching treatment results in significant improvement
in visual acuity. It is generally believed that the critical
period for visual development in humans ends at the age of 6 to 7 years. Some
eye care professionals believed that amblyopia treatment is effective until 9
or 10 years. The American academy of ophthalmology preferred practice pattern
for amblyopia recommends treatment up to age 10 years15.
Oliver
et al16 reported that children older than 8 years showed a
significant improvement in their visual acuity, almost as good as that in
younger children. Rutstein and Fuhr17 reported that age above 8
years, visual acuity of 6/12 or better could be obtained in only 27% of
patients. However, in this study visual acuity of 6/12 or better could be
obtained in 30% of patients older than 8 years.
Epelbaum
et al18 reported that the results of patching therapy could be
observed best when patching treatment is done before three years of age in
strabismic amblyopia. Rutstein et al19 reported that the visual
acuity improvement is somewhat lesser in patients older than seven years than
in younger patients. However, In this study there was a child aged 8 years presented
with anisometropia, best corrected visual acuity 6/24 after giving patching
trial of 6 hours, visual acuity improved to 6/12 and then after six months
reached to 6/7.5 .Visual improvement initially was faster in the patching
group, but after six months analysis the difference of both patching group was
small.
Various studies have favored amblyopia treatment at the age < 6
– 7 years20,21 but few studies have reported better outcomes in
older children22,23. This study results showed that the visual
outcomes were independent of the patient's age, suggesting that the amblyopia
can be treated successfully beyond the age that is considered to be the
critical period for the visual development.
Increased
prevalence of blindness in the population is still a reality in this part of
the world. One way of preventing future blindness is to detect amblyopia at an
early stage and give adequate patch treatment. This could be done by school
health care, at eye clinics, in the local health center, thus preventing blindness
for a low cost.
The limitations of the study
include smaller sample size and shorter follow-ups.
CONCLUSION
This
study concludes that the improvement of vision after three months of initial patching
treatment was comparatively greater than further 3 months of patching (at the
end of 6 months) among patients with strabismic and anisometropic amblyopia.
Author’s Affiliation
Ms. Sumaira
Amir
Optometrist and
Orthoptist
Combined
Military Hospital (CMH), Rawalpindi-Pakistan
Dr. Aamir Asrar
MBBS, MRCOphth, FRCS, Fellowship in Vitreo-Retinal
Surgery, Fellowship in Corneo-Refractive Surgery, Chief Consultant
Ophthalmologist, Amanat Eye Hospital, Islamabad–Pakistan.
Dr. Mubashir Jalis
MBBS, MCPS, FCPS, Fellow-ship in Pediatric Ophthalmology,
Associate Professor Islamabad Medical and Dental Hospital, Consultant Ophthalmologist,
Amanat Eye Hospital, Rawalpindi-Pakistan
Ms. Sadaf Ishtiaq
Optometrist and Orthoptist, MSPH,
Al-shifa school of public health, Rawalpindi-Pakistan
Ms. Bisma Ikram
Optometrist
and Orthoptist, MSPH,
Amanat
Eye Hospital, Rawalpindi-Pakistan
Ms. Sumaira Amir
Concept,
Research Design, Sample collection, Data Collection, Manuscript Writing and data
analysis.
Dr. Aamir Asrar
Sharing
of data and Manuscript Review.
Dr. Mubashir Jalis
Sharing
of data.
Ms. Sadaf Ishtiaq
Data analysis.
Ms. Bisma Ikram
Data analysis.
REFERENCES
1. De Zarat BR, Tejedor J. Current concepts in the management
of amblyopia. Clin Ophthalmol. 2007; 1: 403-14.
2. Stewart CE, Moseley MJ, Stephens DA,
Fielder AR, the MOTAS cooperative. The treatment dose-response in amblyopia
therapy: results from the monitored occlusion treatment of amblyopia study (MOTAS)
Invest
Ophthalmol Vis Sci. 2004; 45: 3048-54.
3. Astle AT, McGraw PV, Webb BS.
Can human amblyopia be treated in adult hood. Strabismus. 2011; 19: 99-109.
4. Repka MX, Beck RW, Holmes JM,
et al. Pediatric Eye Disease Investigator Group. A randomized trial of patching
regimens for treatment of moderate amblyopia in children. Arch Ophthalmol.
2003; 121: 603–611.
5. Scheiman
MM, Hertle RW, Beck RW, et al.; Pediatric Eye Disease Investigator Group.
Randomized trial of treatment of amblyopia in children aged 7 to 17 years. Arch Ophthalmol. 2005; 123: 437–447.
6. Levi
DM. Prentice award lecture 2011: removing the brakes on plasticity in the
amblyopic brain. Optom Vis Sci.
2012; 89: 827–838.
7. Scheiman, M. M. et al. Randomized trial of treatment of
amblyopia in children aged 7 to 17 years. Arch Ophthalmol. 2005;
123: 437–447.
8. Huang,
C. B., Zhou, Y. & Lu, Z. L. Broad
bandwidth of perceptual learning in the visual system of adults with
anisometropic amblyopia. Proc Natl Acad Sci USA, 2008; 105: 4068–4073.
9. Levi, D. M. & Li, R. W.
Perceptual learning as a potential treatment for amblyopia: a mini-review. Vision
Res. 2009; 49: 2535–2549.
10. Li, R.
W., Ngo, C., Nguyen, J. & Levi, D. M. Video-game play induces plasticity in the visual system of adults with
amblyopia. PLOS Biology, 2011;
9: 7339-750.
11. Stewart CE, Moseley MJ, Stephens DA, et al. Treatment dose-response in amblyopia
therapy: the monitored occlusion treatment of amblyopia study (MOTAS).Invest Ophthalmol Vis Sci. 2004; 45: 3048-54.
12. Newsham D. Parental non-concordance with
occlusion therapy. Br J Ophthalmol. 2000; 84: 957-62.
13. Stewart
CE, Stephens DA, Fielder AR, et al. Objectively monitored patching
regimens for treatment of amblyopia: randomised trial. BMJ 2007; 335: 707.
14. Loudon SE, Fronius M, Looman CWN, et al. Predictors and a remedy for Non-compliance
with amblyopia therapy in children measured with the occlusion dose monitor. Invest Ophthalmol Vis Sci. 2006; 47: 4393-400.
15. Amblyopia Preferred Practice Pattern,. American Academy of Ophthalmology, San Francisco, California; Sept
2012.
16. Oliver M, Neumann R, Chaimovitch Y, Gottesman
N, Shimshoni M. Compliance and
results of treatment for amblyopia in children more than 8 years old. Am J
Ophthalmol. 1986; 102: 340–345.
17. Rutstein
RP, Fuhr PS. Efficacy and stability of amblyopia therapy. Optom Vis Sci. 1992;
69: 47–54.
18. Epelbaum
M, Milleret C, Buisseret P, Dufier JL. The sensitive period for strabismic
amblyopia in humans. Ophthalmology. 1993; 100: 323–7.
19. Rutstein
RP, Fuhr PS. Efficacy and stability of amblyopia
therapy. Optom Vis Sci. 2003; 69: 747–54.
20. De Zarate BR, Tejedor J. Current concepts in the management of
amblyopia. Clin Ophthalmol 2007; 1:403-14.
21. Astle
AT, McGraw PV, Webb BS. Can human amblyopia be treated in adulthood. Strabismus.
2011; 19: 99-109.
22. Wallace
DK; Pediatric Eye Disease Investigator Group, Edwards AR, Cotter SA, Beck RW, Arnold RW, Astle WF, et al. A randomized trial
to evaluate 2 hours of daily patching for strabismic and anisometropic
amblyopia in children. Ophthalmology, 2006; 113: 904-12.
23. Pediatric Eye Disease Investigator Group. Randomized
trial of treatment of amblyopia in children aged 7 to 17 years. Arch Ophthalmol.
2005; 123: 437-47.